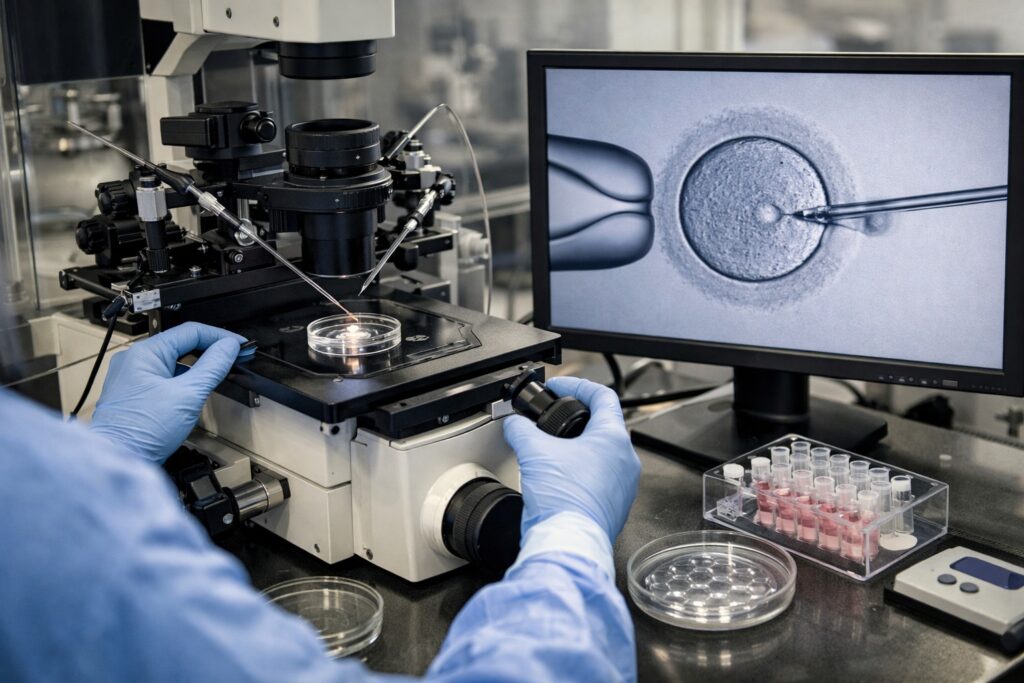
Most articles describe ICSI in one simple line:
A single sperm is injected directly into an egg.
Technically true. But that explanation stops too early.
Because ICSI is not just a lab technique. It’s a clinical decision. And that decision affects biology, treatment cost, risk exposure, and even how future cycles are planned.
If you’re considering ICSI Treatment in Kanpur, especially at an established IVF centre in Kanpur, you need more than a one-line definition. You need to understand what changes, why it’s recommended, and what it means for your specific case.
First, Quick Context (What Everyone Else Covers)
ICSI = Intracytoplasmic Sperm Injection.
It’s a form of ART (assisted reproductive technology), done as part of an IVF cycle.
Instead of placing thousands of sperm around an egg (standard IVF), the embryologist selects one sperm and injects it directly into the egg using a microneedle. That’s the visible part.
The rest — stimulation, egg retrieval, fertilization, embryo culture, transfer — follows the IVF pathway.
Note: If you’re unclear about how IVF itself works, read our IVF treatment breakdown first. ICSI only makes sense when IVF basics are clear.
Why ICSI Was Invented (The Real Reason)
ICSI was developed for severe male factor infertility:
- Very low sperm count
- Poor motility
- Abnormal morphology
- Obstructive azoospermia (sperm retrieved surgically)
Without ICSI, fertilization rates were near zero in these cases. ICSI solved that.
But here’s where things shift.
Today, ICSI is used in far more cycles than medically necessary.
Why? Because clinics fear fertilization failure. And fertilization failure is emotionally devastating. So ICSI became “insurance.”
That assumption needs discussion.
ICSI vs IVF — What Actually Changes
| Standard IVF | Standard IVF |
| Eggs and sperm are placed together | The embryologist chooses the sperm |
| The strongest sperm penetrates naturally | The egg membrane is pierced |
| Biology chooses | The lab chooses |
| Natural selection pressure | Selection pressure bypassed |
So what changes?
Selection pressure.
In IVF, biology chooses. In ICSI, the lab chooses.
That’s not automatically bad. But it matters.
Who Really Needs ICSI (And Who Probably Doesn’t)
Clear Indications:
- Severe male factor infertility
- Previous IVF fertilization failure
- Surgically retrieved sperm (TESA / PESA / micro-TESE)
- Very low egg number (when losing eggs to failed fertilization is risky)
Grey Zone Cases:
- Mild male factor
- Unexplained infertility
- Advanced maternal age
- PGT cycles (many clinics use ICSI routinely here)
Not Ideal:
Couples with completely normal sperm parameters and no prior fertilization failure.
Here’s the uncomfortable truth:
ICSI does not increase pregnancy rates in couples with normal sperm.
It only increases fertilization rates. That’s different.
What the ICSI Process Looks Like (Clinically)
The external process is IVF:
- Ovarian stimulation
- Monitoring
- Trigger injection
- Egg retrieval
Then the lab takes over.
Inside the Embryology Lab:
- Eggs are stripped of surrounding cells
- Maturity is checked
- A single motile sperm is immobilized
- The sperm is injected into the egg cytoplasm
- Eggs are monitored for fertilization (2 pronuclei check)
After that, embryo culture continues as usual. Then embryo transfer or freezing.
Important: ICSI doesn’t guarantee good embryos. It only guarantees fertilization attempt.
Success Rates — What They Don’t Clarify
Many sites say: “ICSI success rate is X%.”
That’s misleading.
There are 3 different metrics:
| Metric | What ICSI Does |
| Fertilization rate per injected egg | ✅ Improves this |
| Blastocyst formation rate | ❌ Does not automatically improve |
| Live birth rate per transfer | ❌ Does not automatically improve |
ICSI improves the first. It does not automatically improve the last two.
If egg quality is poor, ICSI won’t fix that. If sperm DNA fragmentation is high, ICSI may bypass natural barriers — but embryo quality can still suffer.
This is where couples get confused.
Advanced Section 1: Sperm DNA Fragmentation — The Hidden Variable
Most blogs skip this.
If sperm DNA fragmentation is high:
- Fertilization may occur
- Early embryo development may look normal
- But implantation may fail
- Or early miscarriage may occur
ICSI does not repair DNA damage. It just ensures entry.
In fact, because natural selection barriers are bypassed, ICSI may allow genetically weaker sperm to fertilize.
That’s why sperm DNA testing becomes important in repeated failures.
Advanced Section 2: Egg Damage Risk (Rare, But Real)
During ICSI:
- The egg membrane is pierced
- Internal pressure changes
- Mechanical trauma can occur
Not every egg survives injection.
Degeneration rates vary between labs (usually 5–15%). Patients are rarely told this clearly.
Why this matters:
If you have only 3 mature eggs, losing even one matters.
Which is why lab expertise is not a small detail. It’s central.
Advanced Section 3: Is ICSI Overused?
Yes. In many regions.
Why?
- Defensive medicine
- Fear of fertilization failure
- Lab workflow standardization
- PGT requirement (to avoid sperm contamination)
But overuse has trade-offs:
| Trade-off | Impact |
| Higher cost | Increases financial burden |
| More lab manipulation | More handling = more risk |
| No proven benefit | In non-male factor cases |
| Slightly increased risk | Of imprinting disorders (rare, but documented) |
It’s not dangerous. But it’s not neutral either.
Decision should be indication-based.
What Happens If ICSI Fails?
Three possible failure points:
| Failure Point | Next Steps |
| No fertilization | Check egg maturity, sperm viability, activation issues |
| Poor embryo development | Consider egg quality, DNA fragmentation, stimulation protocol |
| Implantation failure | Think uterine factors, endometrial receptivity, immune or hormonal balance |
That’s why repeating ICSI blindly is not strategy. It’s looping.
Risks — For Mother and Baby
For the Mother:
- Same risks as IVF stimulation
- Ovarian hyperstimulation syndrome (OHSS)
- Egg retrieval complications (rare)
For the Baby:
- Slightly higher risk of certain rare genetic conditions
- Slight increase in congenital anomalies (absolute risk still low)
Important nuance:
Many of these risks may be linked to underlying male infertility, not the ICSI procedure itself.
Correlation ≠ causation.
But patients deserve the full picture.
Does ICSI Increase Twin Risk?
No.
Multiple pregnancy risk depends on:
- Number of embryos transferred
- Not the fertilization technique
If single embryo transfer is done, twin risk is low.
When ICSI Isn’t the Answer
Hard truth.
- If egg quality is severely compromised, ICSI cannot fix cytoplasmic aging
- If sperm carries severe chromosomal defects, ICSI cannot correct that
- If uterine environment is hostile, ICSI cannot force implantation
Sometimes couples escalate technology when what’s needed is diagnosis refinement.
Long-Term Considerations Most Blogs Skip
- Repeated ICSI cycles increase financial and emotional fatigue
- Lab dependency increases — outcomes become lab-quality sensitive
- Future male offspring of severe male factor cases may inherit infertility patterns
Not guarantees. But part of informed decision-making.
Cost — What Actually Drives It
ICSI cost is not just “IVF + add-on.”
It includes:
- Micromanipulation equipment
- Skilled embryologist time
- Higher lab handling intensity
- Often bundled with advanced culture techniques
So… Should You Choose ICSI?
Decision Logic:
| Your Situation | ICSI Recommendation |
| Severe male factor | ✅ Yes. Strongly indicated |
| Previous IVF fertilization failure | ✅ Yes |
| Surgically retrieved sperm | ✅ Yes |
| Normal sperm, first cycle | ⚠️ Discuss. Not automatic |
| Doing PGT | ⚠️ Often recommended, but understand why |
Ask your clinic one question:
“What specific factor in our case makes ICSI necessary?”
If they can’t answer clearly, pause.
What Competitors Don’t Tell You — And Why It Matters
They explain the procedure. They list benefits and risks. They show step-by-step timelines.
But they rarely discuss:
- Selection pressure bypass
- DNA fragmentation implications
- Overuse trends
- Failure analysis logic
- Long-term genetic considerations
- Lab skill variability
Because those require nuance. And nuance doesn’t fit into clean marketing pages.
Final Thought
ICSI is powerful. Sometimes life-changing.
But it is not “advanced IVF.” It is a tool.
Use it when the problem is fertilization. Not when the problem is somewhere else.
If you’re exploring this option, don’t stop here.